Spinal Stenosis Surgery Success Rates Explained
Living with spinal stenosis can gradually limit independence, reduce mobility, and undermine confidence. Persistent leg pain, numbness, or weakness often make even simple activities feel exhausting or unsafe. Many patients reaching this point are searching for one clear answer: does spinal stenosis surgery really work, and what are the true surgery success rates?
For patients exploring advanced spine care with specialists such as Dr. Max Greig, an internationally trained orthopedic surgeon known for compassionate, patient-centered treatment, understanding realistic outcomes is essential. Surgery can be life-changing for the right candidate, but success depends on many interconnected factors.
This guide takes a closer look at outcomes, recovery expectations, and patient satisfaction with spinal stenosis surgery, helping you make an informed and confident decision.
What Is Spinal Stenosis and Why Surgery Is Considered
Understanding Spinal Stenosis
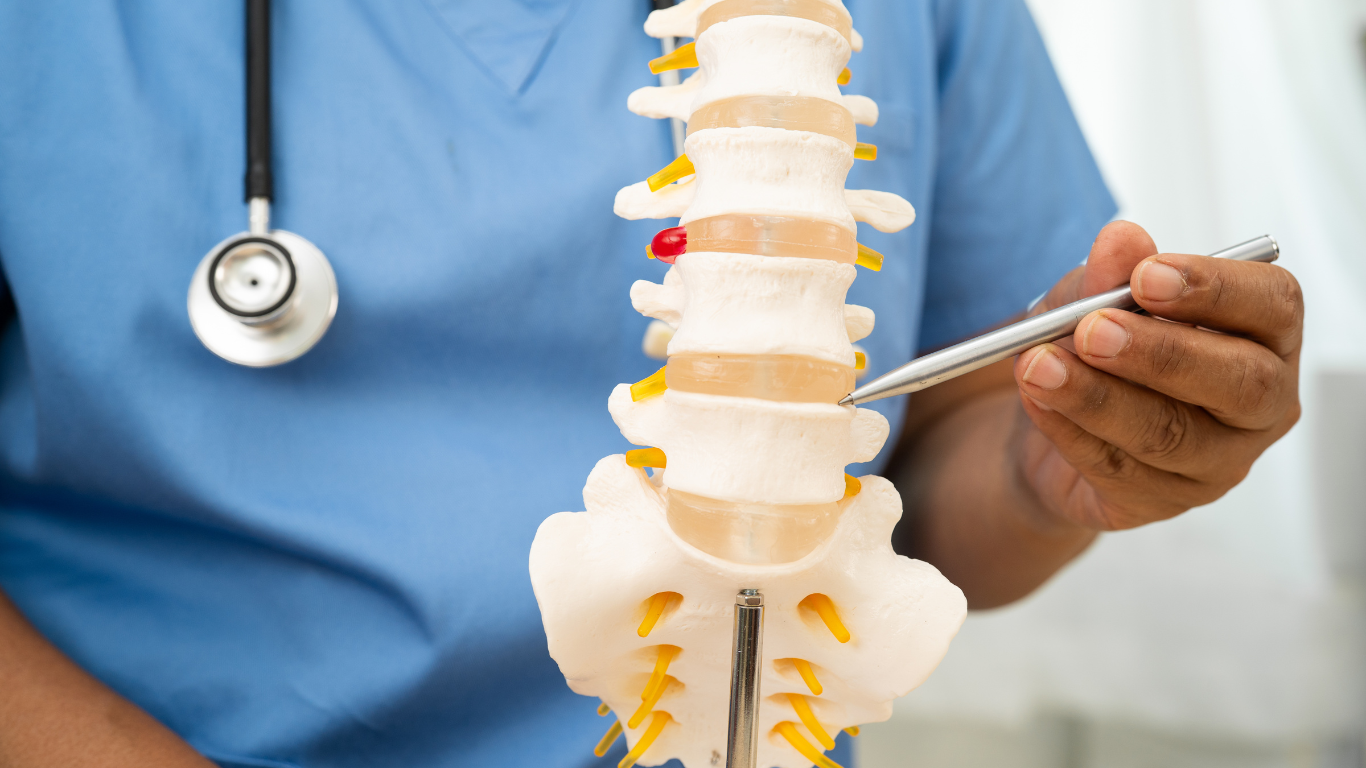
Spinal stenosis occurs when the spinal canal narrows, placing pressure on the spinal cord or nerve roots. This narrowing is most commonly caused by age-related degeneration, arthritis, disc bulges, thickened ligaments, or bone spurs. The lumbar spine is most frequently affected, though cervical stenosis can also cause serious symptoms.
As nerve compression increases, patients may experience worsening leg pain, cramping while walking, numbness, tingling, balance issues, or weakness. When conservative treatments fail to control symptoms, surgery becomes a meaningful option.
When Non-Surgical Care Is No Longer Enough
Physical therapy, medications, injections, and lifestyle changes often help in early or moderate cases. However, once walking distance declines, nerve pain becomes constant, or neurological symptoms progress, delaying surgery can reduce eventual surgery success rates. Timely intervention, when nerve damage is still reversible, improves outcomes and long-term function.
You might be interest in: When Is Back Surgery the Right Choice?
What Do Surgery Success Rates Really Mean?
Defining Success for Spinal Stenosis Surgery
Unlike a simple lab result, surgical success is multi-dimensional. For spinal stenosis, success typically includes pain relief, improved walking tolerance, better balance, restored nerve function, and overall quality of life improvement. Many patients also measure success by reduced medication use and the ability to return to daily activities.
Clinically, surgeons evaluate complication rates, reoperation rates, functional scores, and patient satisfaction surveys. From the patient’s perspective, success is often defined by freedom of movement and reduced fear of pain.
Short-Term vs. Long-Term Outcomes
- Short-term outcomes focus on early recovery, complication rates, and immediate symptom relief within weeks to months.
- Long-term outcomes track durability over years, including recurrence of symptoms or need for additional surgery. High-quality spinal stenosis surgery aims to deliver strong results in both timelines.
Spinal Stenosis Surgery Success Rates by Procedure
Reported success rates are derived from multiple clinical studies and randomized trials summarized in evidence-based guidelines from organizations such as the North American Spine Society (NASS), American Spine Registry and so on.
Lumbar Decompression Surgery Outcomes
Lumbar decompression procedures, such as laminectomy or laminotomy, are among the most common treatments for spinal stenosis. When nerve compression is clearly identified, success rates typically range between 70% and 85% for meaningful improvement in pain and function.
Patients often report increased walking distance, reduced leg pain, and improved balance. Outcomes are strongest when surgery targets specific compressed levels rather than extensive multilevel degeneration without clear symptoms.
Decompression With Fusion: When Stability Is an Issue
In cases involving spinal instability, spondylolisthesis, or deformity, decompression may be combined with spinal fusion. Fusion success depends heavily on bone quality, smoking status, and surgical technique. Fusion-related surgery success rates commonly fall between 70% and 80% for well-selected patients.
While fusion can increase recovery time, it may provide better long-term stability and reduce recurrence of nerve compression in appropriate cases.
You might be interest in: Why Choose Puerto Vallarta for Orthopedic Surgery
Minimally Invasive Spine Surgery Results
Minimally invasive approaches aim to reduce muscle disruption, blood loss, and hospital stay. For eligible patients, these techniques can deliver comparable or better outcomes than open surgery, with faster recovery and lower infection risk. Surgeon experience plays a major role in maximizing success with these methods.
Factors That Influence Surgery Success Rates
Patient Health and Lifestyle
Overall health significantly affects surgical outcomes. Conditions such as diabetes, obesity, osteoporosis, and smoking increase complication risk and slow healing. Patients who optimize nutrition, control blood sugar, and stop smoking before surgery experience higher surgery success rates and faster recovery.
Age alone is not a limiting factor. Many patients over 65 achieve excellent outcomes when their general health is optimized and the surgical indication is clear.
Severity and Duration of Symptoms
Earlier intervention often leads to better results. Chronic nerve compression lasting years can cause permanent nerve damage, limiting recovery even after technically successful surgery. Patients with progressive weakness or worsening walking ability benefit most when surgery is not excessively delayed.
Surgeon Experience and Precision
Surgeon expertise is one of the strongest predictors of outcome. High-volume spine surgeons with advanced training consistently report lower complication rates and better functional outcomes. Careful preoperative imaging, precise decompression, and thoughtful decision-making all contribute to higher success rates.
Postoperative Care and Rehabilitation
Surgery is only one part of the recovery journey. Structured rehabilitation, early mobilization, and adherence to postoperative guidance significantly improve long-term results. Patients who actively engage in physical therapy regain strength faster and report higher satisfaction.
You might be interest in: Why Experience in Orthopedic Surgery Matters for Outcomes
Patient Satisfaction After Spinal Stenosis Surgery
Quality of Life Improvements
Most successful surgeries deliver meaningful improvements in daily living. Patients often report walking longer distances, sleeping better, and participating more fully in family and social activities. Reduced dependence on pain medication is another major contributor to satisfaction.
Managing Expectations
While surgery can relieve nerve compression, it does not reverse arthritis or aging. Patients who understand realistic goals tend to report higher satisfaction. Clear communication between surgeon and patient before surgery is essential for aligning expectations with likely outcomes.
Realistic Concerns
Common Surgical Risks
As with any surgery, spinal stenosis procedures carry risks including infection, bleeding, blood clots, and nerve irritation. Fortunately, serious complications are uncommon when surgery is performed in modern facilities by experienced teams.
Failed Back Surgery Syndrome
A small percentage of patients experience persistent pain after surgery. This can result from scar tissue, incomplete decompression, or unrelated pain sources. Thorough evaluation and careful patient selection significantly reduce this risk.
Revision Surgery Outcomes
Revision surgery generally has lower success rates than first-time procedures. This underscores the importance of accurate diagnosis, precise surgical planning, and choosing the right surgeon from the start.
You might be interest in: Recovery Time for Lumbar Spinal Stenosis Surgery: What to Expect
Choosing Surgery Abroad and Its Impact on Success Rates
Many patients consider spinal stenosis surgery outside their home country to access expert care without long wait times or excessive costs. When performed in accredited facilities with internationally trained surgeons, outcomes can match or exceed those seen in higher-cost healthcare systems.
Physicians like Dr. Max Greig, who combine advanced orthopedic expertise with personalized care and modern surgical standards, attract patients seeking both high-quality outcomes and a supportive recovery environment.
FAQ: Spinal Stenosis Surgery Success Rates
Is spinal stenosis surgery worth it?
For patients with confirmed nerve compression and failed conservative treatment, surgery often provides significant pain relief and improved mobility, making it highly worthwhile.
How long do results from spinal stenosis surgery last?
Many patients experience lasting benefits for years. Long-term success depends on overall spinal health, lifestyle choices, and adherence to rehabilitation.
What is the average recovery time after spinal stenosis surgery?
Initial recovery typically takes six to twelve weeks, with continued improvement over several months. Minimally invasive techniques may shorten this timeline.
Can spinal stenosis return after surgery?
While surgery relieves current compression, degeneration can continue at other levels. Maintaining strength, flexibility, and a healthy weight reduces future risk.
Lumbar Stenosis Surgery: Everything You Need To Know
Making a Confident Decision About Surgery
Understanding surgery success rates empowers patients to move forward with clarity rather than fear. Spinal stenosis surgery, when carefully indicated and expertly performed, offers strong odds of pain relief, improved function, and renewed independence.
Outcomes are best when patients are well informed, medically optimized, and supported by experienced surgical teams.
For individuals seeking transparent guidance, personalized care, and world-class orthopedic expertise, working with a specialist like Dr. Max Greig provides not only technical excellence but also reassurance throughout the entire journey.
With the right preparation and expectations, spinal stenosis surgery can be a powerful step toward living fully again.